Does dietary fiber contain anything of nutritional value? No, it doesn’t. Zero vitamins… Zero minerals… Zero protein… Zero fat… Nothing, zilch, not even digestible carbohydrates. Why, then, is it considered a healthy nutrient? As the story goes, you can thank Dr. John Harvey Kellogg for that:
“Dr. Kellogg was obsessed with chastity and constipation. True to principle, he never made love to his wife. To “remedy” the sin of masturbation, he advocated circumcision without anesthetic for boys, and mutilation of the clitoris with carbolic acid for girls. He blamed constipation for “nymphomania” in women, and lust in men, because, according to Kellogg, impacted stools inside one’s rectum were stimulating the prostate gland and the female vagina into sexual proclivity.” [
link]
To fix these “ailments,” Dr. Kellogg was prescribing a coarse vegetarian diet along with 1 to 3 ounces of bran daily, and mineral oil with every meal. As any nutritionist will tell you, the decline of libido and infertility are among the very first symptoms of malnutrition prevalent among ardent vegans. And in this particular case, extra bran and mineral oil were “enhancing” damage by blocking the assimilation of nutrients from an already meager diet.
And what was Dr. Kellogg’s rationale for prescribing mineral oil? Well, because so much fiber was enlarging stools, intense straining was required to expel them. The oil was used as a lubricant to reduce pain caused by straining, and to prevent bloody anal fissures inside the anal canal.
However, the ultimate fame and money came to Dr. Kellogg not from crusading against sex, but from ready-to-eat morning cereals after he found that baking bran into cereals proved to be incredibly profitable for Kellogg Company. From that point on, it took another sixty years or so of relentless brainwashing to turn what once used to be a dirt-cheap livestock feed into a premium health food.
Well, that’s
an old story, and I can understand if you doubt it—it sounds too incredulous to be true! So, let’s debunk fiber’s mythology with facts and science. Here we go, one myth at a time:
Myth #1: For maximum health, obtain 30 to 40 g of fiber daily from fresh fruits and vegetables.
Reality: Here is how many fresh fruits you’ll need to eat throughout the day in order to obtain those 30 to 40 grams (1-1.4 oz.) of daily fiber:

As you can see, that comes to five apples, three pears, and two oranges. A small apple contains 3.6 g of fiber and 15.5 g of sugars. A small pear—4.6 g and 14.5 g; and a small orange—2.3 g and 11.3 g, respectively (USDA National Nutrient Database; NDB #s: 09003; 09200; 09252 [
link]).
These ten small (not medium or large) fruits will provide you with 36.4 g of indigestible fiber and a whopping 143.6 g of digestible sugars, or an equivalent of that many (ten) tablespoons of plain table sugar!
And that‘s before accounting for all the other carbs consumed throughout the day for breakfast, lunch, dinner, and from snacks and beverages.
So ask yourself this question: even if you are a 100% healthy 25-year-old muscle-bound athlete, would you ever ingest that much sugar willingly? Well, maybe under the influence of a controlled substance or torture…
But that’s exactly what’s being recommended for “health purposes” to children and adults. It‘s not surprising that so many Americans are suffering from the ravages of diabetes and obesity—a moderately active adult can utilize no more than about 200 grams of carbohydrates per day without encountering a scourge of the inevitable obesity, prediabetes, or diabetes.
The ratio of digestible carbohydrates (sugars) to fiber in vegetables, cereals, breads, beans, and legumes is, on average, similar to fruits. Thus, no matter how hard you try to mix’n’match, you’ll be getting harmed all the same.
Please do note that if you are healthy, active, and normal weight, there is nothing wrong with consuming fruits and vegetables in moderation. The point of this section is to impress on you that it is NOT OK to binge on fruits to ingest recommended daily intake of fiber.
This myth—that fruits and vegetables are the best source of dietary fiber—is probably the most pervasive and damaging of all. If 30 grams of fiber is what you’re really after, you’re better off getting it from supplements. These, after all, have almost no digestible carbs. But, then, of course, you run into those other persistent falsehoods…
Myth #2: Fiber reduces blood sugar levels and prevents diabetes, metabolic disorders, and weight gain.
Reality: That’s a blatant deception. If you consume 100 g of plain table sugar at once, the blood absorbs all 100 g of sugar almost as soon as it reaches the small intestine, where the assimilation takes place. If you add 30 g of fiber into the mix, the fiber may extend the rate of sugar assimilation into the blood, from, let‘s say, one hour to three.
But at the end of those extra three hours the blood will still absorb exactly the same 100 g of sugar—not an iota more, not an iota less. If you are a diabetic, the only difference will be that you‘ll require more extended (long-acting) insulin for type 1 diabetes, or larger doses of medication for type 2 diabetes in order to deal with slow-digesting sugars, and your blood glucose test will not spike as high after the meal.
But you‘re fooling no one but a glucose meter. In all other respects, the damage will be all the same, or even worse. And that‘s even before taking into account the negative impact of fiber on the digestive organs, or hyperinsulinemia and triglycerides on the heart, blood vessels, and blood pressure.
Myth #3: Fiber-rich foods improve digestion by slowing down the digestive process.
Reality: Fiber indeed slows down the “digestive process,” because it interferes with digestion in the stomach and, later, clogs the intestines the “whole nine yards.” The myth is that it can be good for health and the digestive process.
Here is what you get from delayed digestion: indigestion (dyspepsia), heartburn (GERD), gastritis (the inflammation of the stomach‘s mucosal membrane), peptic ulcers, enteritis (the inflammation of the intestinal mucosal membrane), and further down the chain, constipation, irritable bowel syndrome, ulcerative colitis, and Crohn‘s disease.
All this, in fact, is the core message of
Fiber Menace: fiber slows down the digestive process! And slow digestion is ruinous for your health. Don‘t mess with fiber unless your gut is made of steel!
Myth #4: Fiber speeds food through the digestive tract, helping to protect it against cancer.
Reality: Not true. In fact, this claim directly contradicts the claim that fiber-rich foods slow down the digestive process. For a reality check, here’s an excerpt from a college-level physiology textbook that reveals the truth:
“Colonic Motility: Energy-rich meals with a high fat content increase motility [the rate of intestinal propulsion]; carbohydrates and proteins have no effect.”
R.F. Schmidt, G. Thews; Human Physiology, 2nd edition. 29.7:730 [link]
This, incidentally, is why low-fat diets and constipation commonly accompany each other. And don’t count on getting any cancer protection from fiber, either. That‘s yet another oft-repeated deception.
Myth #5: Fiber promotes a healthy digestive tract and reduces cancer risk.
Reality: Not true. Here’s what doctors-in-the-know have to say on the subject of the colon cancer/fiber connection:
Lack of Effect of a Low-Fat, High-Fiber Diet on the Recurrence of Colorectal Adenomas
“Adopting a diet that is low in fat and high in fiber, fruits, and vegetables does not influence the risk of recurrence of colorectal adenomas.”
Arthur Schatzkin, M.D et al. The New England Journal of Medicine; [link]
The excerpt below comes, of all places, from the Harvard School of Public Health:
Fiber and colon cancer
“For years, Americans have been told to consume a high-fiber diet to lower the risk of colon cancer—mainly on the basis of results from relatively small studies. Larger and better-designed studies have failed to show a link between fiber and colon cancer.”
Fiber: Start Roughing It [link]
Not convinced yet? Well, here is even more damning evidence from the U.S. Food and Drug Administration:
Letter Regarding Dietary Supplement Health Claim for Fiber With Respect to Colorectal Cancer
“Based on its review of the scientific evidence, FDA finds that (1) the most directly relevant, scientifically probative, and therefore most persuasive evidence (i.e., randomized, controlled clinical trials with fiber as a test substance) consistently finds that dietary fiber has no [preventive] effect on incidence of adenomatous polyps, a precursor of and surrogate marker for colorectal cancer; and (2) other available human evidence does not adequately differentiate dietary fiber from other components of diets rich in foods of plant origin, and thus is inconclusive as to whether diet-disease associations can be directly attributed to dietary fiber. FDA has concluded from this review that the totality of the publicly available scientific evidence not only demonstrates lack of significant scientific agreement as to the validity of a [preventive] relationship between dietary fiber and colorectal cancer, but also provides strong evidence that such a relationship does not exist.”
U. S. Food and Drug Administration – Center for Food Safety and Applied Nutrition Office of Nutritional Products, Labeling, and Dietary Supplements; [link]
Alas, the story doesn’t end there. Adding insult to injury, Chapter 10 of my book entitled
Fiber Menace,
“Colon Cancer” cites studies that demonstrate the connection between increased fiber consumption and colon cancer. Also, countries with the highest and lowest consumption of meat are compared. Not surprisingly, the countries with the lowest consumption of meat and, correspondingly, the highest consumption of carbohydrates, including fiber, have the highest rate of digestive cancers, particularly of the stomach.
Myth #6: Fiber offers protection from breast cancer.
Reality: A blatant, preposterous lie. According to the recent massive study jointly conducted by the U.S. Center for Disease Control and Prevention, the Ministry of Health of Mexico, and the American Institute for Cancer Research, it’s the opposite: women with the highest consumption of carbohydrates, and, correspondingly, of fiber, had the highest rates of breast cancer:
Carbohydrates and the Risk of Breast Cancer among Mexican Women
“In this population, a high percentage of calories from carbohydrate, but not from fat, was associated with increased breast cancer risk.”
Isabelle Romieu, et al; Cancer, Epidemiology, Biomarkers & Prevention; 2004 13: 1283–1289. [link]
Although this study has singled out carbohydrates as the culprit behind various cancers, where there’s smoke, there’s also fire: carbs and fiber are as inseparable as Siamese twins, as I have already explained in Myth #1.
Myth #7: Fiber lowers blood cholesterol levels, triglycerides, and prevents heart disease.
The myths about fiber’s role in coronary heart disease (CHD) and the management of elevated cholesterol have their roots in some dubious research, which culminated in “reduced mineral absorption and myriad of gastrointestinal disturbances” after the study participants were given supplements containing a mixture of guar gum, pectin, soy fiber, pea fiber, and corn bran along with a low-fat and reduced cholesterol diet.
The total reduction of LDL cholesterol after 15 weeks was from “7% to 8%”. As any cardiologist will tell you, the reduction of “bad” cholesterol from, let’s say, 180 to 166 mg/dL (-8%) is completely meaningless. Besides, if you cause someone to have a “myriad of gastrointestinal disturbances” in the process, that person is more likely to die prematurely from malnutrition and cancer than of stroke or heart attack.
Even then, this marginal reduction of cholesterol had little to do with fiber, and everything to do with the reduction of dietary fats. LDL cholesterol happens to be a major precursor to bile. The moment a person is placed on a low-fat diet, their cholesterol level drops because their liver no longer needs to produce as much bile.
In addition, intestinal inflammation caused by soluble fiber blocks the ability of bile components to get absorbed back into the bloodstream, further lowering the cholesterol level. This is as basic as the physiology of nutrition gets, and it makes the whole claim of a fiber-cholesterol connection a deliberate con.
There is another dimension to the con used to “prove” fiber‘s role in reducing cholesterol. Most of the studies on fiber’s cholesterol-lowering effect—particularly psyllium—used The American Heart Association’s (AHA) Step 1 diet.
The Step 1 diet is high in carbohydrates and low in fat by design, with less than 10% of total energy derived from saturated fat. During clinical studies among people using the Step 1 diet without added fiber, their total cholesterol fell by 8%, LDL cholesterol fell by 6%, and HDL cholesterol fell by 16%.
In other words, the Step 1 diet on its own, without any extra fiber and/or digestive side effects, demonstrates an almost identical drop in cholesterol as with added fiber. In legalese, this particular “coincidence” is called fraud, plain and simple.
So one fraud more, one fraud less…what‘s the worry, if my cholesterol goes down?
Well, there is a legitimate worry, at least, according to this respected source:
Problem with American Heart Association “Step 1″ diet
“Although the AHA Step 1 diet decreased total and LDL cholesterol levels in this group of women, it decreased HDL cholesterol by an even greater proportion. In women, a low HDL cholesterol concentration is a stronger independent predictor of cardiovascular disease risk than is elevated total cholesterol or LDL cholesterol. Therefore, women who follow AHA guidelines for lowering their serum cholesterol may actually be increasing their risk of heart disease”
Alan R. Gaby, M.D. Townsend Letter for Doctors and Patients [link]
Amazingly, back in 2001, the AHA replaced the Step 1 diet with the Step II, TLC, and ATP III diets [
link], which are even more restrictive in terms of fat, and even more permissive in terms of carbohydrates.
And don’t get me started on triglycerides… First, nothing raises triglycerides as profoundly as a high-fiber diet does, because, paraphrasing the smoke-fire cliché, where there’s fiber, there’re carbohydrates, usually eight to ten times as much.
This fact—the more fiber you consume, particularly from natural sources, the higher your level of triglycerides from carbohydrates intake—has been dodging Dr. Dean Ornish [
link] one of the most prominent proponents of a high-carb/high-fiber diet.
Second, once inside the colon, fiber itself gets fermented by intestinal bacteria. Among the byproducts of bacterial fermentation are short-chain fatty acids—butyrate, acetate, and propionate. Most of these fatty acids get assimilated directly into the bloodstream to provide energy.
According to the
Dietary Reference Intakes manual “current data indicate that the [energy] yield is in the range of 1.5 to 2.5” calories per each gram of consumed fiber [
link]. If you aren’t starving, the absorbed fatty acids unused for energy get metabolized by the liver into triglycerides for further storage as body fat.
Granted, a few calories here, a few calories there, may not seem like a lot. Still, if you are consuming 30 to 40 grams of fiber daily plus whatever “hidden” carbohydrates you are ingesting unknowingly along with processed food, it all adds up to epidemics of obesity, diabetes, and heart disease.
Myth #8: Fiber satisfies hunger and reduces appetite.
Reality: When the scientists from the Human Nutrition Research Center on Aging at Tufts University decided to look at this dubious claim, here is what they have found out:
Fermentable and Nonfermentable Fiber Supplements Did Not Alter Hunger, Satiety or Body Weight in a Pilot Study of Men and Women Consuming Self-Selected Diets
“Despite the large total intakes of FF [fermentable fiber - ed.] and NFF [non-fermetable fiber - ed.] supplements, there were no significant changes in body weight or fat during consumption of either type of fiber, even among the subjects with higher BMI.”
The Journal of Nutrition [link]
And as you keep digging deeper, you soon realize that consuming too much fiber may actually contribute to obesity. Because fiber rapidly absorbs water and expands in the stomach up to five times its original size and weight, it indeed pacifies the appetite for a short while.
Unfortunately, while faking satiety, expanded fiber also stretches out the stomach‘s chamber, and each new fill-up requires progressively more and more fiber to accomplish the same trick. Lo and behold, in order to reduce its capacity and “speed up” satiety, surgeons suture the stretched-out stomachs of obese individuals or squeeze them with a bridle (LAP-BAND©). A complete opposite of what fiber does.
Myth #9: Fiber prevents gallstones and kidney stones.
Reality: I‘ve seen several observational studies that claim fiber can prevent gallstones. It isn‘t true. It‘s common knowledge that diabetes and obesity are consistently associated with higher risk for gallstones, and both of these conditions are the direct outcome of excessive consumption of carbohydrates, and correspondingly, of fiber. Beyond these few studies, there isn‘t a shred of physiological, anatomical, clinical, or nutritional evidence that connects gallstone formation with fiber consumption.
Here‘s an excerpt from
Fiber Menace that sheds further light on the gallstone-fiber connection:
Fiber’s affect on the small intestine: Not welcome at any price
Gallstones are formed from concentrated bile salts when the outflow of bile from the gallbladder is blocked. […] before they can form, something else must first obstruct the biliary ducts. Just like with pancreatitis, that “something” is either inflammatory disease or obstruction caused by fiber.
Women (in the West) are affected by gallstones far more than men, because they are more likely to maintain a “healthy” diet, which nowadays means a diet that is low in fat and high in fiber. Since the gallbladder concentrates bile pending a fatty meal, no fat in the meal means no release of bile. The longer the concentrated bile remains in the gallbladder, the higher the chance for gallstones to form (from bile salts).
Fiber Menace, page 25 [link]
Just as with gallstones, kidney stones are also common among people who suffer from diabetes and obesity, because excessive consumption of carbohydrates increases the excretion of urine, changes its chemistry, and predisposes to kidney stones.
To investigate this myth further, I consulted
PubMed, a service of the National Library of Medicine, which is the most thorough compendium of medical research. I reviewed eighty-one articles published between 1972 and 2005 (the year I was researching my book) that mention the words “fiber” and “kidney stones”. Not a single one of them connected kidney stones to fiber consumption, while several specifically pointed out that an increased consumption of carbohydrates is one of the major contributing factors.
One article suggested that a diet free of digestible carbs, but containing fiber, makes urine composition less stones-prone. You don‘t have to be Dr. Watson to deduce that fiber—an indigestible substance—can‘t materially affect urine chemistry, because what can‘t get digested also can‘t reach the kidneys. Besides, it wasn’t the presence of fiber that did the “trick,” for those investigators, but the reduction in digestible carbohydrates.
Myth #10: Fiber prevents diverticular disease.
For a while, it was difficult to disprove this absurdity by appealing to common sense. So I devoted a whole chapter in
Fiber Menace to explaining why fiber CAUSES diverticular disease. Thank God, I am no longer alone in this thinking:
Fiber Not Protective Against Diverticulosis
Contrary to popular medical wisdom, following a high-fiber diet has no protective effect against developing asymptomatic diverticulosis, according to a colonoscopy-based study presented at the 2011 Digestive Disease Week (DDW) meeting (abstract 275). In fact, the study showed that patients who ate more fiber actually had higher prevalence of the disease.
Gastroenterology and Endoscopy News, July 2011, Volume: 62:07 [link]
Fiber May Not Prevent Diverticular Disease
For decades, doctors have recommended high-fiber diets to patients at risk for developing the intestinal pouches, known as diverticula. The thinking has been that by keeping patients regular, a high-fiber diet can keep diverticula from forming. But the new study suggests the opposite may be true.
WebMD, January 23, 2012 [link]
A High-Fiber Diet Does Not Protect Against Asymptomatic Diverticulosis
A high-fiber diet and increased frequency of bowel movements are associated with greater, rather than lower, prevalence of diverticulosis. Hypotheses regarding risk factors for asymptomatic diverticulosis should be reconsidered.
Gastroenterology; Volume 142, Issue 2, Pages 266-272.e1, Feb. 2012 [link]
The only problem with all of the above research is that it may take another six to eight years to tell people what I was telling them eight years ago: if you wish to protect your gut from diverticular disease, keep fiber out of it.
Myth #11: Fiber is safe and effective for the treatment and prevention of diarrhea.
Reality: Actually, it’s the complete opposite—fiber, particularly soluble, is the most common cause of diarrhea in children and adults. That’s why it’s recommended as a laxative to begin with. The idea of fiber as a preventive treatment for diarrhea is one of the most preposterous and harmful fiber-related frauds.
Soluble fiber is widely present in fruits, vegetables, laxatives, and processed foods, such as yogurt, ice cream, sour cream, cream cheese, soy milk, non-dairy creamers, preserves, jellies, candies, cakes, snack bars, canned soups, frozen dinners, sauces, dressings, and endless others.
It’s always expertly concealed from scrutiny behind obscure names such as agar-agar, algae, alginate, β-glucan, cellulose gum, carrageen, fructooligosaccharides, guaran, guar gum, hemicellulose, Irish moss, kelp, lignin, mucilage, pectin, oligofructose, polydextrose, polylos, resistant dextrin, resistant starch, red algae, and others.
These inexpensive industrial fillers are added as stabilizers and volumizers to practically all processed foods, because they hold water, maintain shape, and fake “fattiness.” Besides, they are cheaply bought by the ton, and are resold retail by the gram for immense profit.
Once inside the body, these fiber fillers remain indigestible, hold onto water just as tight, and prevent absorption. This property—the malabsorption of fluids—lies behind soluble fiber‘s laxative effect: under normal circumstances a very limited amount of fluids enter the large intestine. When their amount exceeds the colon’s holding capacity, you get hit with diarrhea.
In other words, the term “laxative” is just a euphemism for a “diarrheal” agent. If you overdose on a fiber laxative, you’ll end up with diarrhea. If you “overdose” on fiber from food, you’ll end up with exactly the same diarrhea. But since fiber in food can’t be measured as reliably as fiber in capsules, wafers, or powders, it’s much easier to “overdose” the latter fiber and cause severe diarrhea.
Besides, fiber is even more offensive than synthetic laxatives, because the byproducts of its fermentation cause intestinal inflammation, flatulence, bloating, and cramping—just as described in medical references:
Malabsorption Syndromes
Colonic bacteria ferment unabsorbed carbohydrates into CO2, methane, H2, and short-chain fatty acids (butyrate, propionate, acetate, and lactate). These fatty acids cause diarrhea. The gases cause abdominal distention and bloating.
Gastrointestinal Disorders; The Merck Manual of Diagnosis and Therapy [link]
The diarrheal effect of soluble fiber is particularly harmful for children, because their smaller intestines need lesser amounts to provoke diarrhea. According to the Centers for Disease Control and Prevention:
The Management of Acute Diarrhea in Children
…diarrhea remains one of the most common pediatric illnesses. Each year, children less than 5 years of age experience 20-35 million episodes of diarrhea, which result in 2-3.5 million doctor visits, greater than 200,000 hospitalizations, and 325-425 deaths.
Centers for Disease Control and Prevention [link]
These figures are from 1992, the latest statistic I could find. It must be much worse today because fiber is so much more prevalent. And if you analyze the most basic facts, you’ll understand immediately why this travesty is taking place. Consider this:
A single adult dose of Metamucil®—a popular fiber laxative made from psyllium seed husks—contains 2 g of soluble fiber in 6 capsules [
link]. One apple, one orange, and one banana—not an unusual number of fruits a child may eat throughout the day—contain a total 4 g of soluble fiber, or an equivalent of 12 capsules of Metamucil for a much larger adult.
And that’s on top of all the juices, cereals, yogurts, ice creams, candies, cakes, and all other processed food consumed on the same day, all loaded with fiber as well. No wonder that “diarrhea remains one of the most common pediatric illnesses” in the United States, and there is an acute shortage of pediatricians nationwide.
Myth #12: Fiber relieves chronic constipation.
I left this myth for last because it is the most pervasive. For the same false reasons that people believe in the cleansing prowess of fiber, everyone and their uncle also believes that fiber relieves constipation.
Not quite true. According to the experts from the American College of Gastroenterology’s Functional Gastrointestinal Disorders Task Force, all legitimate clinical trials “…did not demonstrate a significant improvement in stool frequency or consistency when compared with placebo.” [
link]
In plain English, it means fiber is no better at relieving constipation than a sugar pill. Indeed, how could it be, when fiber causes constipation in the first place! Again, I describe the exact reasons behind the fiber-constipation connection in
Fiber Menace.
Even The Merck Manual of Diagnosis and Therapy, the very first book your doctor consults when needing up-to-date medical advice, has recently changed their tune regarding fiber, clearly the outcome of my work.
“Fiber supplementation is particularly effective in treating normal-transit constipation but is not very effective for slow-transit constipation or defecatory disorders” [
link]
In plain English, it means the following: “Fiber supplements will catapult healthy people into a loo because of their laxative effect. But for anyone with a history of chronic constipation, they don’t work.”
Finally, consider the stern warnings, that accompany Metamucil, a fiber supplement made from psyllium:

So not only do fiber supplements not work for most people with chronic constipation, but they may also make them ill. Probably not ill enough to kill their libido as Dr. Kellogg originally intended, but imagine enjoying sex with your partner while being bloated and flatulent courtesy of extra fiber in your morning cereals.
That doesn’t describe a health food, does it?
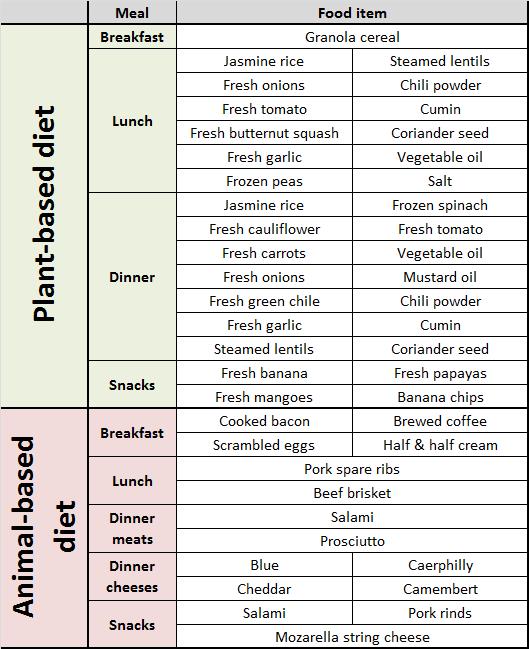
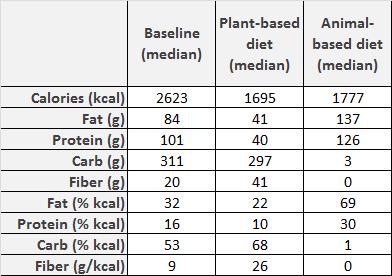
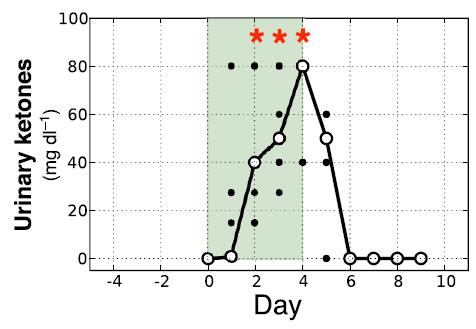



 Today’s article is a guest post from Konstantin Monastyrsky of
Today’s article is a guest post from Konstantin Monastyrsky of 

